What You Need to Know About Breast Implant Illness and My Opinion on BII
- Posted on: Mar 21 2019
Breast Implant Illness, or BII, is one of the hottest topics in plastic surgery today.
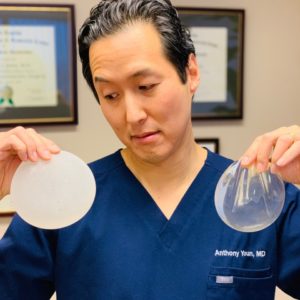 Breast implant illness refers to a constellation of symptoms that some women appear to develop after undergoing breast augmentation with implants. These symptoms include fatigue, muscle and joint pain, brain fog, fevers, rashes, and hair loss. Until recently, there have been no large scale scientific studies that have proven its existence. However, over the past several years, thousands of women have come forward on social media and online to share their stories of breast implant illness, and their often improvement of their symptoms once their implants are removed.
Breast implant illness refers to a constellation of symptoms that some women appear to develop after undergoing breast augmentation with implants. These symptoms include fatigue, muscle and joint pain, brain fog, fevers, rashes, and hair loss. Until recently, there have been no large scale scientific studies that have proven its existence. However, over the past several years, thousands of women have come forward on social media and online to share their stories of breast implant illness, and their often improvement of their symptoms once their implants are removed.
Unfortunately, there is a big disconnect between mainstream plastic surgery and breast implant illness groups. I find it sad and disappointing that there appears to be a big gulf between plastic surgeons, whom I believe the vast majority are doing what they believe is best to make their patients happy, and patients who have real problems after getting breast implants.
I hear stories of plastic surgeons who blow off their patients’ symptoms and concerns, which I don’t think is right. I also have had patients come to see me in consultation who have asked for what I consider very invasive, extreme operations on their breasts.
So going forward, I hope that I can help shine a light on this very real subject and maybe even help form a bridge to the thousands of women who are having autoimmune and other symptoms that they attribute to their breast implants.
Studies that show no link between implants and connective tissue disease / symptoms:
- 1998 Study from Sweden – 10,000 women – no evidence of association between women with breast implants and connective tissue disease
- 2001 Study from Denmark – 11,000 women – no difference in rates of rheumatic conditions between women with breast implants and without
- 2003 Study from Denmark – 238 women – no connection found in women with breast implants for connective tissue disease or other symptoms
- FDA Core and Post Approval studies in US
- Mentor Memory Gel Implants – 1000 women – 64% follow up at 7 years – At 10 years 97.6% of women are happy they made decision to have breast implants
- Natrelle Study – 715 women – 65%+ follow up at 10 years – 93% satisfaction at 10 years
Studies that show a link between breast implants and connective tissue disease / symptoms:
- 1993 – J Autoimmunity – Looked at 46 women with breast implant concerns to 45 women without implants. Statistically significant incidence of antibodies to collagen in women with silicone breast implants.
- 1997 – Annals of Allergy Asthma Immunology – Compared the cellular immune responses of 23 women with silicone breast implants to 26 women without, finding an increased frequency of cellular immune responses to collagen in the women with silicone breast implants.
- 2011- ASIA identified – autoimmune syndrome induced by adjuvants – pattern of symptoms caused by systemic reaction to adjuvants (like silicone). – Is this a better term for “Breast Implant Illness?”
- 2017 – Immunologic Research – Review of literature to determine if removal of silicone breast implants in people with silicone-related complaints or autoimmune diseases improves their symptoms. They calculated that removal of silicone breast implants improved symptoms in 75% of patients (469 of 622). But in those with autoimmune diseases only 16% (3 of 18) improved.
- 2018 – International Journal Epidemiology – Compared 24,561 women with silicone breast implants to 98,604 women without – found a small, but significant difference in being diagnosed with autoimmune/rheumatic disorders – strongest association is with Sjogren’s Syndrome, Systemic Sclerosis, and Sarcoidosis.
- 2018 – Annals of Surgery – Study out of MD Anderson – Looked at US FDA Breast Implant Postapproval studies – 99,993 patients – Found women with silicone breast implants had a higher rate of Sjogren’s Syndrome, Scleroderma, Rheumatoid Arthritis, and Melanoma. There was also a statistically increased association with neurological disorder, multiple sclerosis, and myositis. BUT silicone implants had statistically decreased rates of fibromyalgia and lung cancer.
- Keep in mind that the individual studies do not show an increased risk of these.
Who may be susceptible to ASIA “breast implant illness?”
- 2013 – Netherlands J Medicine – Invited 80 women who had silicone breast implants and unexplained symptoms to be evaluated. 75% reported pre-existent allergies. After a symptom- free period of years, a pattern of systemic symptoms developed in more than 65% of women – fatigue, myalgia, arthralgia, morning stiffness. In 69% of women, explantation reduced symptoms significantly.
- 2015 – Clinics of Rheumatology – Review of data linking silicone implants to autoimmunity recommended that individuals with previously diagnosed autoimmune disorders or with a genetic preponderance for hyperactive immune system should reconsider silicone breast augmentation.
What do I believe?
I’ve been a private practice plastic surgeon for 15 years, having done thousands of breast implant operations. I have seen a number of patients, some of mine, some of other doctors, who have symptoms that resemble breast implant illness.
 Whenever a patient asks me to remove her implants, whether she has symptoms of BII or not, the answer is always yes. I fully believe that the decision to have implants should be made by the woman with the implants, and no one else.
Whenever a patient asks me to remove her implants, whether she has symptoms of BII or not, the answer is always yes. I fully believe that the decision to have implants should be made by the woman with the implants, and no one else.
Of those patients who’ve had them removed due to concerns that they were causing symptoms or autoimmune disease, unfortunately most of those with autoimmune disease don’t appear to have improved. I would love to say that they get better, but it hasn’t been my experience. They may say they feel somewhat improved, but I have rarely seen a complete resolution of their autoimmune disease.
However, most of them with symptoms, but not true diagnoses of autoimmune disease appear to resolve significantly. I have recently had two patients with these types of symptoms resolve completely after their implants were removed.
I believe Breast Implant Illness is real. I think a better term has been coined by our rheumatology colleagues: ASIA – autoimmune syndrome induced by adjuvants.
This appears to me to be a relatively rare but real constellation of symptoms with the most common being fatigue, joint pain, muscle pain, brain fog, fevers, rashes, and hair loss.
These symptoms may be more common in women who have silicone filled implants over saline implants.
The symptoms don’t necessarily appear to happen immediately, but possibly several years after the operation.
Patients with a past history of allergies or autoimmune disease might be at higher risk of developing these symptoms.
The vast majority of women with breast implants don’t develop this, as evidenced by the large scale studies that don’t support the connection. However, it’s possible that 1% or more may develop these issues.
Therefore, I commend the women who have taken it upon themselves to spread knowledge that breast implant illness is real. They are an important part of the solution and their stories must be heard and shared with plastic surgeons and rheumatologists.
I believe that more studies need to be performed so we can learn as much as we can about breast implant illness.
If you have symptoms of breast implant illness, what is recommended?
The majority of plastic surgeons would probably recommend explantation and removal of the capsule only if it is thickened.
Online breast implant illness groups recommend a complete capsulectomy (removal of the implant and the entire scar tissue capsule surrounding it) or en bloc removal of implants – where the implant and entire capsule (scar tissue shell around the implant) are removed altogether in one piece. The concern is that leaving part of the capsule behind, even if it isn’t thickened, could leave behind substances that can continue to cause the symptoms of breast implant illness. Also, by removing it separately, this could cause some type of contamination of the area.
What do I recommend for my patients?
This is what I am currently recommending for my patients, based off the best information I have at this time. These recommendations may change as new information comes out, and does not necessarily reflect the recommendations of other doctors. It is just what I believe and recommend.
- Happy with breast implants, no symptoms – leave alone.
- Desire to remove breast implants, but no symptoms and no capsule thickening – explantation alone.
- Desire to remove breast implants, but no symptoms, capsule thickened – explantation with partial or full capsulectomy.
- Unhappy with breast implants and symptoms – explantation and full capsulectomy if it can be performed safely.
What I do not recommend at this time:
- en bloc removal of implants – very invasive with large incision/scar – I know there are patients and doctors recommending this extreme operation for women with BII. The idea is that there is no contamination of the implant pocket when the implant is removed. The problem is that this is a pretty extreme operation with long scars. Before I recommend it, I need to see scientific evidence that the benefits of this operation outweigh the drawbacks. At this time, I haven’t been able to find any studies that show this operation should be performed. But I am open minded, and look forward to following future research very closely.
What do I recommend for new patients who want breast implants?
If you can be happy without breast implants, it’s always best to stay natural. Surgery comes with risks, and although the satisfaction rate of breast implants is over 95%, they are not for everyone.
- Smooth walled saline or silicone gel filled implants – not textured due to risks of ALCL
- Implants placed ideally through an incision under the breast and dual plane (below the muscle)
- Inform patients with a history of allergies or autoimmune issues that you may be at higher risk of BII. You may want to consider either saline implants instead of silicone, or to not have the surgery at all.
Tagged with: alcl, Auto Immune Symptoms, BII, brain fog, breast augmentation, Breast Implant Illness, breast implant sickness, breast implants, Breast Implants and ALCL, breast implants and illness, capsulectomy, cosmetic surgery, detroit, Dr. Anthony Youn, dr. youn, en bloc, fatigue, FDA, hair loss, plastic surgery, sickness, silicone breast implants, silicone illness
Posted in: Plastic Surgery News

